Insist on including cardiac diagnostic imaging as part of your child's next sick visit!
RISE IN PEDIATRIC MYOCARDITIS COVID-19 MYOCARDITIS STANDARDIZED DIAGNOSTICS ▪ Heart MRI (Cardiac MRI). A cardiac MRI shows your heart's size, shape and structure. This test can show signs of inflammation of the heart muscle. [10] ▪ Electrocardiogram (ECG or EKG). This quick and painless test shows your heart's electrical patterns and can detect irregular heartbeats. [11] ▪ Chest X-Ray: An X-ray image shows the size and shape of your heart, as well as whether you have fluid in or around the heart that might be related to heart failure. [12] ▪ Blood Tests: There are no specific blood tests to confirm the diagnosis of myocarditis; however, an otherwise unexplained elevation in troponin (a blood test that indicates heart muscle damage) and/or electrocardiographic features of cardiac injury are supportive [13]. Blood tests for Troponins (proteins in the blood which are released when the heart muscle has been damaged), BNP (a blood test that measures levels of a protein that is made by your heart and blood vessels.) [14]
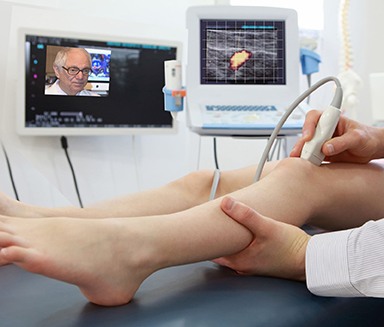
▪ Doppler Ultrasound for Acute Myocarditis: Another diagnostic solution that's made available for bedside imaging of poor cardiac contractility from myocarditis and pericardial effusion is the use of a Point of Care Ultrasound. Case reports demonstrate the estimation of left ventricular function abnormalities [15]. Other advanced studies employing Contrast-enhanced ultrasound and molecular imaging have been used to can detect endothelial inflammation in the left ventricle [16]. ▪ Cardiovascular MR Elastography (MRE): Classical MRE uses an external mechanical transducer to assess the viscoelastic properties of cardiac soft tissues which is technically difficult in an MR suite due to probe placement and ECG lead distribution. Using the wave genereted by the valve closure is now possible. [17*] ▪ Ultrasound Elastography: Elastography for tissue plasticity has been used worldwide for 15 years and recent studies have reported myocardial stiffness expressed in kilopascal (kPa) instead of shear wave velocity. Vibrations related to aortic valve closure generated MR detectable data allowing clinical data at multiple depths in the pediatric patient which was difficult in the adult subject. [18*][19*] |
|
In Feb. 2022, lead directors of The AngioFoundation, The NY Cancer Resource Alliance and publishers of PREVENTION101.org forged a collaborative outreach community project with the For Elysa Foundation (myocarditis awareness org) to form a national coalition of clinical support associations, research foundations, researchers and parent groups dedicated to the awareness of rare pediatric diseases and critical disorders. This collective concept called "MOMMIES ON A MISSION" is a unique and remarkable platform that aspires to support the many pediatric disorders that plague today's children. Known as 'Project One", Mommies on a Mission will launch the ONE VOICE crusade to leverage new awarness response for the deadly health threat of Myocarditis in America's children. "MOMMIES ON A MISSION" is a creative title Mrs. Jana Rojas (director of For Elysa Foundation) used to describe her fellow advocates who, like her, established a dedicated benevolent program to battle pediatric myocarditis through education, awareness and to support clinical research. Even more are driven to forge standardized screening of myocarditis as part of a national prevention and early detection initiative. "Losing another child to this terrible and insidious disease is one child too many! It's time we joined hands with all groups, legislators, medical societies and anyone who can make a difference. We hope to deploy a multi-stage battle plan to address this disease and enact new solutions in every pediatrician's office!", states Dr. Noelle Cutter (Molloy College, NY Cancer Resource Alliance).
|
|
BDI partners with most qualified pediatricians and other specialists who tend to the many diagnostic needs of children. Through the power of the digital ultrasound platform, our growing community of TELEMED PARTNERS (ranging from medical practitioners, pain healers, specialists and health centers) now support the positive use of collaborative communication and imaging technologies to widen their ability to help our common young patients. Creating a united alliance of like-minded caregivers have helped assemble the information that we now have to help one another with their patients and ours. Together, we aspire to offer more ways for patients to get access to the help they need while employing efficient and safer alternatives to receiving professional health care. See Feature article. See Feature article |
|
REFERENCES: |
| Disclaimer & Copyright Notice: Unless otherwise indicated on this Internet web site, you may display, download, archive, and print a single copy of any information on this Internet web site, or otherwise distributed from us for such personal, non-commercial use. Also, certain content may be licensed from third-parties. The licenses for some of this Content may contain additional terms. When such Content licenses contain additional terms, we will make these terms available to you on those pages, in the Terms of Use or in the Additional Information section of our Site (which his incorporated herein by reference). This website does not support, endorse or recommend any specific products, tests, physicians, procedures, treatment opinions or other information that may be mentioned on this site. Referencing any content or information seen or published in this website or shared by other visitors of this website is solely at your own risk. The publishers/producers of this Internet web site reserves the right, at its sole discretion, to modify, disable access to, or discontinue, temporarily or permanently, all or any part of this Internet web site or any information contained thereon without liability or notice to you. |