A SENSIBLE SOLUTION FOR EARLY DETECTION OF DENSE BREASTSWritten by: Dr. Robert L. Bard
WHO NEEDS A DENSITY SCAN? INDEX AREA OF SUSPICION DIAGNOSTIC IMAGING STRATEGY FROM SCAN TO TREATMENT SCANNING INNOVATION:
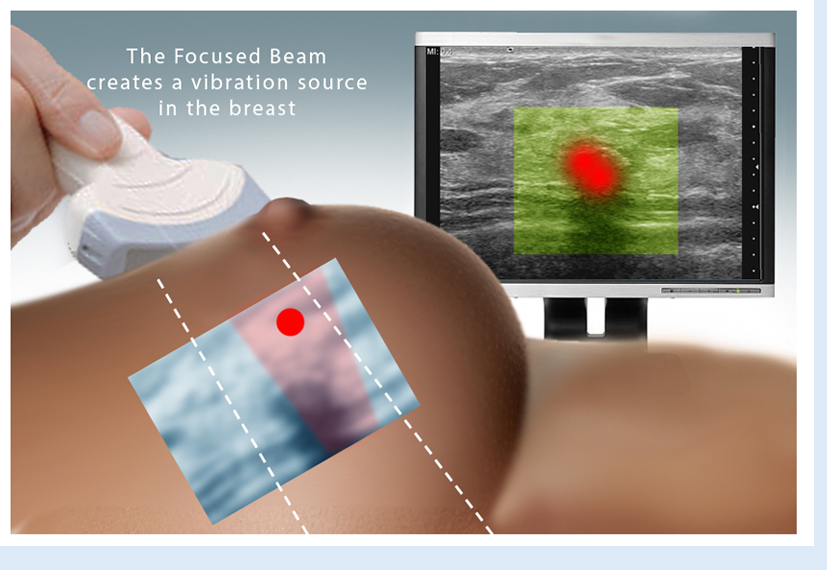
Hybrid imaging refers to combining diagnostic modalities to assess disease and monitor therapy. A useful combination of options is the tumor vessel flow density to assess aggression and treatment progress. Similarly, tissue elastography is useful for border detection of malignant masses.
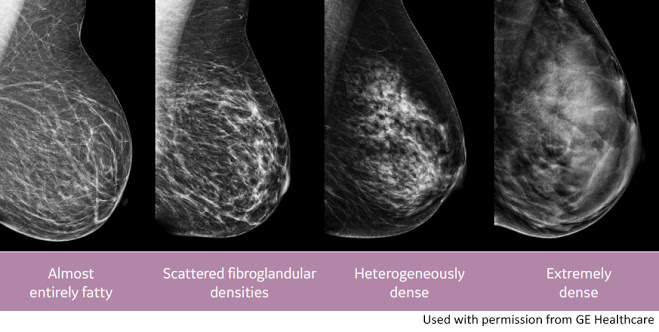
THE DENSE BREAST SCAN MOVEMENT The 1st World Conference of Breast Ultrasound in Philadelphia (1979) recognized ultrasound superiority in dense breast diagnostics but the density level was never quantified until recently. Mammography assessment of breast density is graded into four categories. Mammographers readily admit that these levels are subjective at best and technical factors such as mammary tissue compression and x-ray voltage/amperage dramatically influence the darkness or whiteness of the image • Where is Ultrasound most useful? • What is Doppler sonogram technology? • What is 4D volumetric density histogram imaging? • How is 3D/4D Doppler imaging used? • Can a negative test be used to reduce biopsies?
|
||||||||||||||
What Does It Mean to Have Dense Breasts?Source: CDC.gov A mammogram shows how dense your breasts are. When you get the results of your mammogram, you may also be told if your breasts have low or high density. Women with dense breasts have a higher risk of getting breast cancer. PARTS OF THE BREAST BREAST CANCER RISK: Women with dense breasts have a higher chance of getting breast cancer. The more dense your breasts are, the higher your risk. Scientists don’t know for sure why this is true. Breast cancer patients who have dense breasts are not more likely to die from breast cancer than patients with non-dense (fatty) breasts.
|
||||||||||||||
| * * * SAVE THE DATE * * * |
|
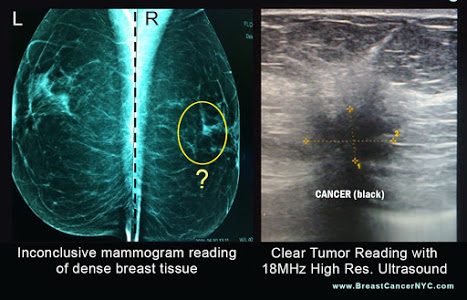
On July 27-29, Bard Diagnostic Imaging is offering a comprehensive DENSE BREAST SCREENING DAY, employing an array of imaging advancements dedicated to the visibility of dense breast tissue and cancer early detection. This special program is dedicated to supporting dense breasted patients by first identifying one's actual breast density (through a density assessment scan) to establish a base line for the full diagnostic study (est. 15-20 minutes per patient). For those with any level of breast density, a major concern is the rate of possible cancers that may be missed from to potential misreadings of a mammogram. It is clinically imperative to have a second opinion with the breast sonogram in areas that are more suspicious. A second look of the dense breast area with 3D scanning technology consists of two parts: first is the regular 3D electronic sweep, which gives you a volumetric tissue study. The next is the 4D real-time automated scan, which focuses on the area of concern and the most dense part of the tissue. Mammogram imaging tends to represent dense tissue as "white" as it also does a small tumor (associate this with a "Polar Bear in a Snowstorm"). Medical interpreters look upon the white tissue as the area where mammograms could miss looming cancers. This is where the 3D and 4D ultrasound imaging comes in; we can now read the density of the tissue which aligns with the potential risk of cancer and navigate through and around the breast giving us the ability to disseminate tissue from tumor. (Read about the data and elevated risk of cancer in dense breasted patients in cancer.org). Through the latest imaging innovation, we have the means to quantify and mitigate this risk by detecting and identifying the "white level" and scanning with the computerized analysis of the volume of suspicious tissue. Make an appointment today @ 212-355-7017. Slots are limited. |
||
| BACK TO HOME PAGE | |||
|
|||||||||||||||||
FAQ about Non-Invasive Sonic Technology & the Future of Cancer Biopsies Since 1973, Dr. Bard established global recognition in the medical field through his contributions in the advancement of cancer diagnostic innovations. His special use of advanced imaging technologies are widely praised as the painless alternative and a more accurate innovation as well as a much faster solution for acquiring results over surgical biopsies. For the patient, it's a world of difference and immediate peace of mind when the 3D imaging establishes the diagnosis during the examination as you literally see the pictures in front of you in real time. Q: How accurate is Advanced Sonography in identifying cancers? (open) Q: Give us an example of your 4D Scan's accuracy over conventional diagnostic methods? (open) Q: What types of cancers are most commonly captured with this technology? (open) Q: How can digital scanning be instrumental in Early Detection? (open) Q: What are the benefits of using the Doppler Ultrasound imaging for BREAST CANCER? (open) Q: Why scan the lymph nodes in the axillae? (open) Q: What are the most recent upgrades in the cancer imaging industry? (open) Q: Can this technology be useful in other health issues and disorders? (open)
|
|||||||||||||||||
 |
|||||||||||||||||
|
COMPUTERIZED 3D DOPPLER HISTOGRAM ANALYSIS
For more information or to subscribe to our EARLY CANCER DETECTION & PREVENTION PROGRAM newsletter, contact Bard Cancer Diagnostics today at: 212.355.7017 - or email us at: bardcancercenter1@gmail.com. Bard Cancer Diagnostics is located at 121 E. 60th St. Suite #6A New York, NY 10022. Visit the complete website: www.CancerScan.com
|
EARLY DETECTION SAVES LIVES!
|
 |



 BREAST CANCER SCREENING REGIMEN
BREAST CANCER SCREENING REGIMEN


 As of Jan '18, Dr. Robert Bard spearheaded a partnership with a host of cancer educators, medical practitioners and non-profit foundations (allied under
As of Jan '18, Dr. Robert Bard spearheaded a partnership with a host of cancer educators, medical practitioners and non-profit foundations (allied under